Giant cell arteritis is the most common primary systemic vasculitis in adults. Current literature estimates that approximately one-third of patients with GCA have PMR at presentation. The term “temporal arteritis” began to gain popularity in the 1930s and was further linked to other inflammatory and rheumatological diseases such as polymyalgia rheumatica (PMR) by Jennings in 1938. The pathology of the disease was further explained by Gilmoure in 1941 when he described the presence of giant cells as part of the disease. At the time, the disease was known as “Horton’s disease”. Horton and his team were the first to perform a temporal artery biopsy and describe the now well-known histopathological findings of granulomatous vasculitis. Their presentations included systemic symptoms such as fever, weakness, headache, pain, and difficulty chewing, as well as ophthalmologic symptoms of transient diplopia and vision loss. Then in 1932, Bayard Horton reported two patients presenting with symptoms that would eventually be highly characteristic of giant cell arteritis. Hutchinson described these findings as “thrombotic arteritis of the aged.” At the time, there was no known link between atherosclerosis/arteriolosclerosis and this arteritis. Hutchinson was treating an 80-year-old patient who had been experiencing “painful red streaks” on his head that were so uncomfortable he was unable to wear his hat. The next time GCA is noted was in the English literature in 1890 by Jonathan Hutchinson. He noted that “these diseased conditions may terminate in loss of sight.” In his observations, he suggested excising the temporal arteries in order to treat these patients and save their vision. He had discussed a potential relationship between inflamed arteries and visual signs and symptoms. The earliest observation was recorded by an ophthalmologist named Ali Ibn Isa al-Kahhal. References to GCA can be found dating all the way back to 10th century Baghdad. This review serves to highlight the essential concepts in our current understanding of the management of patients with GCA. There is a significant amount of research and discussion regarding the underlying etiology, pathogenesis, and appropriate management of patients with GCA. When GCA is suspected, treatment with corticosteroids is indicated on an urgent basis, as further vision loss and fellow eye involvement are usually preventable. Since the vision loss from AAION can progress rapidly, and can involve the fellow eye within a matter of days, GCA is considered an ophthalmologic emergency. The most commonly feared sequela of GCA is permanent visual loss secondary to arteritic anterior ischemic optic neuropathy (AAION). In addition to vision loss, patients commonly note associated symptoms such as headache, jaw claudication, diplopia, myalgias, and constitutional symptoms. Since patients with GCA often present with vision loss, ophthalmologists are on the front lines of diagnosing the disorder. Based on United States census data from 2000, the prevalence of GCA is approximately 160,000. The condition is also known as temporal arteritis. Histopathologically, GCA is marked by generalized granulomatous inflammation of medium- to large-sized vessels that occurs in the elderly. Retinitis pigmentosa-this is a group of diseases that causes retinal degeneration and a gradual decline in vision.Giant cell arteritis (GCA) is the most common primary vasculitis in adults.Flashes and floaters-vitreous floaters may be a symptom of a detached retina, which requires laser treatment or surgery.Macular holes- macular holes can cause blurred or distorted central vision.Retinal detachments or tears-if the retina is detached from its normal position, it can cause permanent vision loss.It is the most common cause of blindness and vision loss in Australia. Macular degeneration-MD causes damage to the macula which also affects central vision.Diabetic retinopathy-this occurs when the blood vessels in the retina change, affecting central vision. 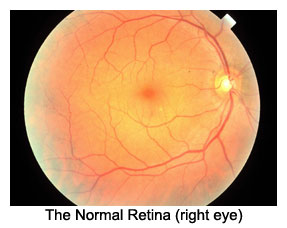
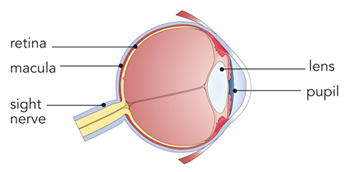
Some of the main retinal diseases that we see in our patients are: PersonalEYES are the eye specialists that can help you with a range of retinal diseases treatment. However, if you are at risk for any retinal disease, you should get regularly tested to maintain the optimal vision for as long as possible. You should always visit your optometrist when you notice any change in vision. These retinal diseases often occur in the back of the eye and are not readily visible, making them more difficult to treat until it’s too late and the damage is irreversible. Retinal Diseases There are a variety of conditions that can affect the vitreous and retina. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
